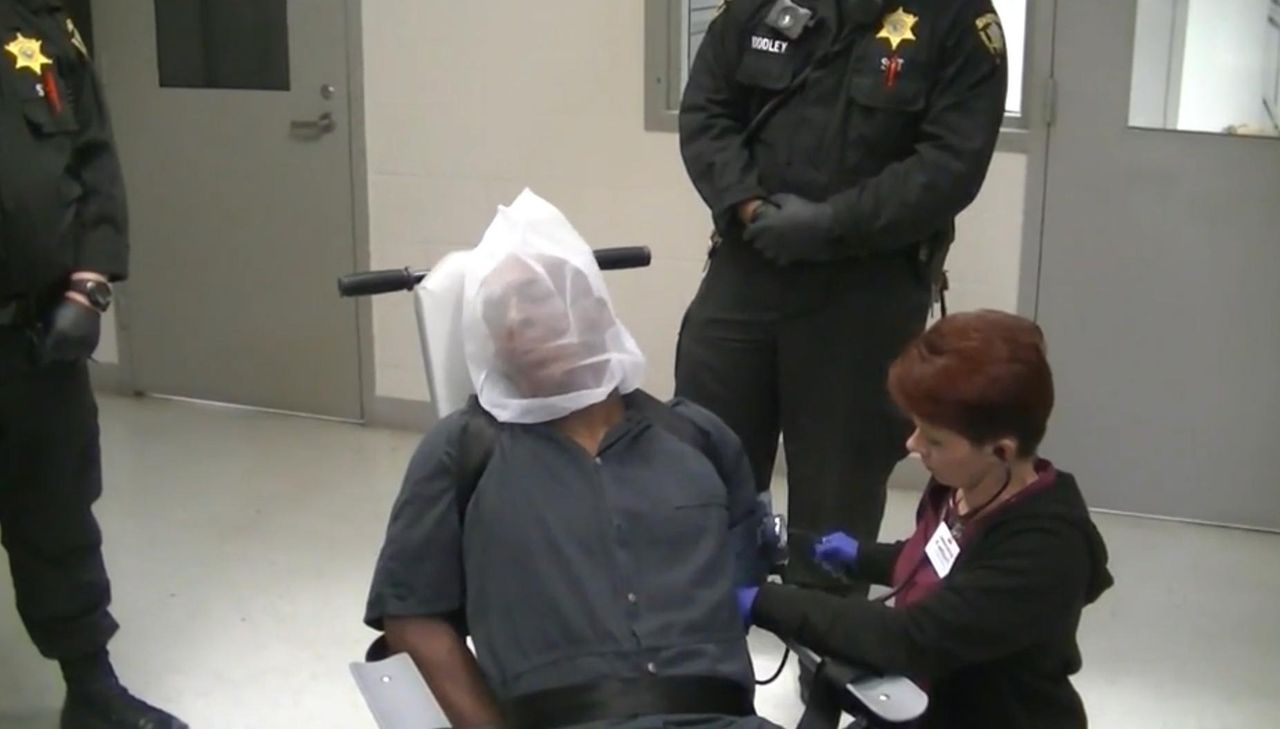
Former county detention center nurse Michelle Heughins is being charged with involuntary manslaughter in connection to the death of John Neville, an inmate at Forsyth County Jail in Winston-Salem, North Carolina. Heughins will plead not guilty when she appears before a judge next month.
So far, she is the only person to have been charged in Neville’s death even though there were several detention officers on hand. And medical providers say only punishing the nurse is unjust.
Neville died after being handcuffed and pressed against the ground while he was experiencing a medical emergency in December 2019, but the staff failed to administer care or take his injuries seriously. A grand jury recently dropped all charges against the five security officers that restrained him, and healthcare professionals are hoping Heughins receives the same treatment.
Michelle Heughins was the only medical provider on the scene when Neville suffered his injuries. She entered the room to find the five officers restraining Neville as he struggled to breathe. Autopsy records show he ultimately died of a brain injury due to cardiac arrest, due to asphyxia during a prone restraint.
John Neville leaves behind one daughter and two sons, Brienn, Kristopher, and Sean Neville.
Neville’s family has since filed a civil lawsuit against the Forsyth County Sheriff’s Office. It alleges that “the detention officers and nurse who purported to assist Mr. Neville altogether failed to recognize the seriousness of his condition or to follow the policies set in place for handling inmates or detainees with serious health problems or who are experiencing a medical emergency.”
Now that the body cam footage has been made public, providers are weighing in on what went wrong.
Shelia, a nurse with over 40 years of experience, reflected on her time as a detention center nurse while reviewing the footage.
“I worked in a prison hospital and a maximum security corrections center about 20 years ago. I’m seeing the same issues now with the Heughins case that I experienced 20 years ago,” she said.
Sheila also discussed the role nurses play in corrections facilities.
“The way it works is the COs [corrections officers] are there to respond to behavior. The medical workers are there to respond to medical. But the two don’t talk to each other, don’t work together. [Mr. Neville] got behavioral response treatment for a medical issue.”
She believes the corrections officers acted inappropriately and should’ve deferred to Heughins when Neville exhibited signs of distress.
“[In the bodycam footage] I didn’t see any correct policies being worked out. I know the officers acted out of their scope of practice. When the nurse arrived, the CO officers are supposed to stand down, but as you see in the video, the COs maintained control. [Heughins] should have assumed it or asked for it, but instead it was the COs making medical decisions.”
“You’re told that the officers are in control of everything,” Shelia continued. “You have to be really tough and experienced to fight to take over. You can’t get intimidated. If I’m the person who has the medical knowledge, then I’m the one who takes the lead in the medical situation. I used to get a lot of heat for that.”
“In the videos you can hear the officers asking [Heughins] to leave the room. How was he [Neville] supposed to get medical attention? Everything the officers were doing was a behavioral response. She was not allowed to follow the standards of care. That’s the main thing that bothers me.”
She also said being the only medical provider can be intimidating when you’re facing a room full of armed corrections officers.
“You can’t be intimidated, and you can’t be afraid, and you really, really have to have working knowledge. If you work corrections, you don’t see situations like this often, maybe once every six months. You need to have a strong and recent experience in the hospital,” she added.
She also blamed the officers on staff for not intervening sooner when Neville started to exhibit signs of asphyxiation.
“The officers are also supposed to know basic first aid, basic CPR. They should have noticed his respirations. Everybody knows this. We all saw what happened to George Floyd. If you have your knee on someone’s belly, on their neck, what do you think is going to happen?”
She said it’s important to treat all prisoners as human beings, regardless of why they ended up in prison.
“I’m a nurse first. You were a murderer, child abuser, I leave that outside. When I go through that door, I am a nurse and they are a patient. I treat them like Mr. President. But that isn’t the dominant culture. Instead, it’s, ‘You’re inmates, you get what you get.’ It may be two weeks before a patient gets their medication, before a patient gets their inhaler. The actual distribution of health care is horrible.”
Erika, an ER nurse from California, also came to Heughins’ defense.
“I think this nurse is a scapegoat for the crimes committed by the officers,” Erika said. “The family wants justice for a wrongful death, and they should get it. The nurse did not restrain the inmate, nor did she hogtie the inmate. Why then is she facing manslaughter charges? To me this looks like excessive force committed by the officers. While the nurse did not strongly object to the officer’s actions, she did not participate in the excessive force herself. Why is this even a case against her?”
She’s seen the same kind of behavior from police officers in the ER.
“I’ve witnessed police officers being too aggressive with patients in emergency departments. It’s very difficult to tell an armed officer to back off when they are subduing a patient (or inmate). I’ve never worked in a jail but I imagine the nurses do not interfere when officers are doing their supposed job.”
“A repeat of George Floyd’s death happens regularly, and something needs to change,” she continued. “Holding a jail nurse responsible for an excessive force death caused by law enforcement will not solve the problem.”
Chanan, another nurse from California, questioned whether Heughins had the proper training for this type of situation.
“She may not have a lot of hospital experience … and if you don’t have the skills and experience in ACLS, it’s not going to be clear how to jump in and what to do,” Chanan said. “There’s a lot of emotion and anxiety in situations like this. I have to presume that she was also witnessing at least the segment before she enters [in the bodycam footage] and initiates resuscitation efforts. I’m sure this wasn’t easy for her.”
But Sheila said that’s not Heughins’ fault.
“If she didn’t have the right experience and training, then this goes back to her employer. A systems issue once again.”