A new study from New York University shows a surprising connection between periodontal disease (gum disease) and Alzheimer’s. Researchers at the NYU College of Dentistry and Weill Cornell Medicine found that older people with more harmful than healthy bacteria in their mouths are more likely to show evidence of amyloid beta in their cerebrospinal fluid (CSF), which is considered a key biomarker for Alzheimer’s disease.
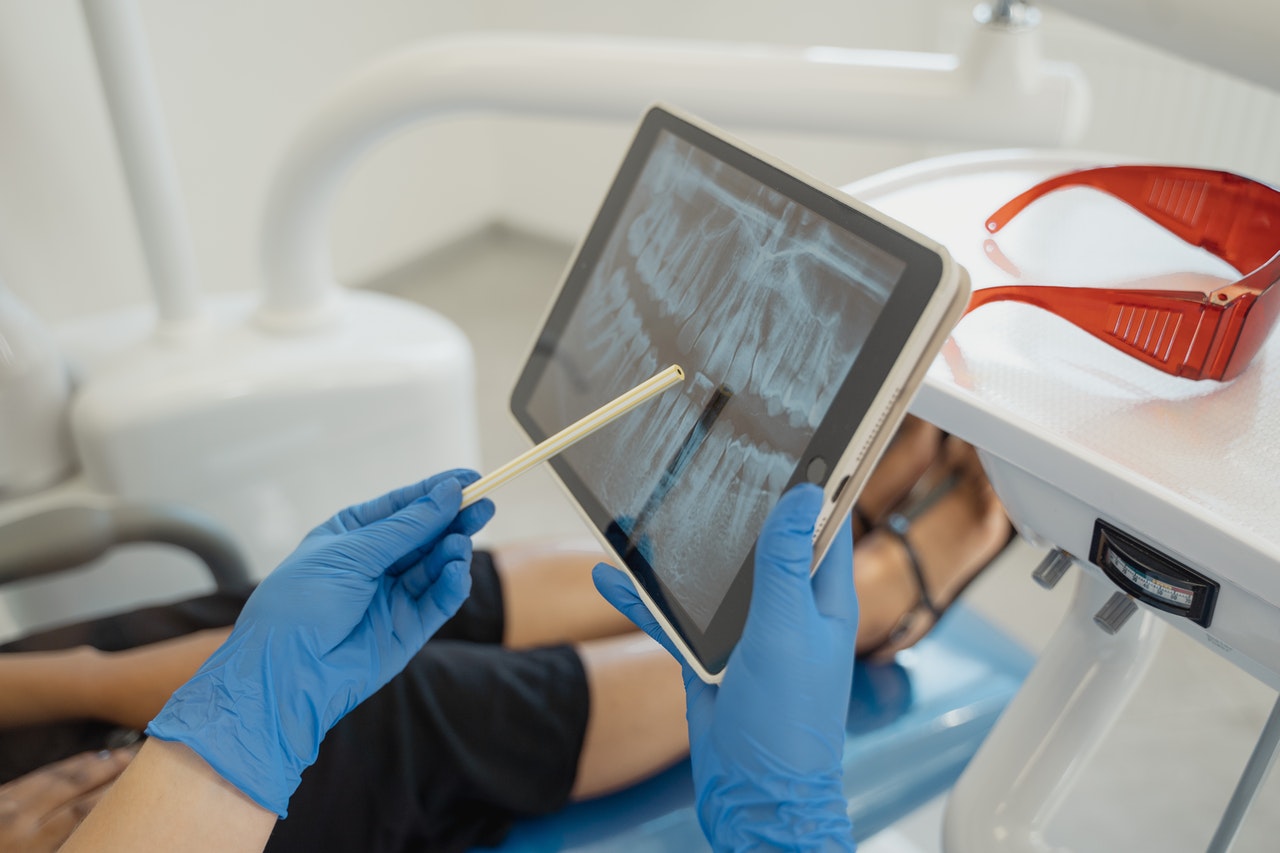
If you want to keep your mind sharp, you might want to visit your dentist.
The Link Between Gum Disease and Alzheimer’s
Published in Alzheimer’s & Dementia: Diagnosis, Assessment & Disease Monitoring, the study is a wake-up call for older adults and their loved ones who may be concerned with potential cognitive decline.
Patients with Alzheimer’s disease have two distinct proteins in their brains: amyloid beta and tau. Amyloid beta clumps together to form plaques and is believed to be the first protein deposited in the brain as the disease develops. Tau builds up in nerve cells and forms tangles that lead to lost connections, inhibiting the person’s memory and other essential functions.
Researchers looked at the mouths of 48 adults ages 65 and up. They collected bacteria from under the gumline and used a lumbar puncture to collect CSF, which they used to determine the levels of amyloid beta and tau. To calculate the person’s risk of Alzheimer’s, they looked for lower levels of amyloid beta, which suggest higher levels in the brain, and higher levels of tau.
They found that individuals with higher quantities of harmful bacteria in the mouth, such as prevotella, porphyromonas, and fretibacterium, compared to healthy bacteria, including corynebacterium, actinomyces, and capnocytophaga, were more likely to have a signature Alzheimer’s CSF, a key indicator of developing the disease.
Senior author Mony J. de Leon, EdD, professor of neuroscience in radiology and director of the Brain Health Imaging Institute at Weill Cornell Medicine, commented on the results:
“The mechanisms by which levels of brain amyloid accumulate and are associated with Alzheimer’s pathology are complex and only partially understood. The present study adds support to the understanding that proinflammatory diseases disrupt the clearance of amyloid from the brain, as retention of amyloid in the brain can be estimated from CSF levels. Amyloid changes are often observed decades before tau pathology, or the symptoms of Alzheimer’s disease are detected.”
While more research is needed to understand the relationship between proinflammatory bacteria and a person’s risk of Alzheimer’s, the results suggest that proper oral health can help build immunity against cognitive decline, but the expression of these proteins involves more than one bacterium.
“Our results show the importance of the overall oral microbiome—not only of the role of ‘bad’ bacteria, but also ‘good’ bacteria—in modulating amyloid levels,” said Angela Kamer, DDS, PhD, associate professor of periodontology and implant dentistry at NYU College of Dentistry and the study’s lead author. “These findings suggest that multiple oral bacteria are involved in the expression of amyloid lesions.”
Historic Findings
The study could be a potential game-changer when it comes to testing for and preventing Alzheimer’s. The CDC says that around 70% of adults over the age of 65 have periodontal disease. 5.8 million Americans reported symptoms of Alzheimer’s in 2020. If the link between the two diseases turns out to be true, these findings could help providers protect their patients from cognitive decline. It may also increase collaboration between dentists and neurologists.
“To our knowledge, this is the first study showing an association between the imbalanced bacterial community found under the gumline and a CSF biomarker of Alzheimer’s disease in cognitively normal older adults,” Kamer added. “The mouth is home to both harmful bacteria that promote inflammation and healthy, protective bacteria. We found that having evidence for brain amyloid was associated with increased harmful and decreased beneficial bacteria.”
However, researchers didn’t see a direct link between gum bacteria and tau levels, so it’s not yet clear if these proteins grow later or if the person will eventually develop symptoms of Alzheimer’s.
The next step is to conduct a longitudinal study and clinical trial where researchers see if regular deep oral cleanings can help modify brain levels of amyloid beta or prevent Alzheimer’s.
The study is an important reminder to keep your teeth clean, even if you aren’t worried about developing Alzheimer’s.